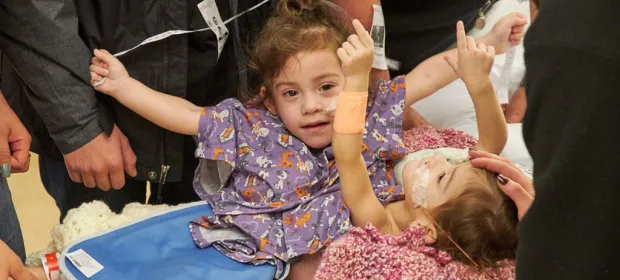
Photo by David Hodges: Two-year-old twin sisters Erika and Eva Sandoval were thoraco-omphalo-ischiopagus
twins, positioned facing each other and joined from the lower chest and upper-abdomen level down.
Stanford Medicine News Center - December 9th, 2016 - by Erin Digitale
Conjoined twins Erika and Eva Sandoval were successfully separated at Lucile Packard Children’s Hospital Stanford in a 17-hour surgery that began Dec. 6 and stretched into the early morning hours of Dec. 7. Prior to separation, the 2-year-old twins of Antelope, California, shared much of their lower body.
“They did very well,” said lead surgeon Gary Hartman, MD, clinical professor of surgery at the School of Medicine. “I’m very pleased with the outcome.”
The Sandoval girls are the seventh pair of conjoined twins Hartman has separated and the fifth separation surgery he has done at Stanford. The last separation at Packard Children’s was performed in 2011.
“It’s amazing how strong these girls are, and it’s amazing what their team performed,” said Aida Sandoval, the twins’ mother. “Seeing them now in the ICU, you look at them and think, ‘You’re missing your other half,’ but we know that this is the right path for them: to be independent, have the chance to succeed and explore on their own everything the world has to offer.”
Erika and Eva are now in stable condition in the pediatric intensive care unit, where they are expected to recover for about two weeks. Their physicians anticipate that the girls will spend an additional two weeks in the hospital before they go home. They are sharing a hospital room but are in separate beds.
Prior to separation, Erika and Eva were thoraco-omphalo-ischiopagus twins, positioned facing each other and joined from the lower chest and upper-abdomen level down. They had separate hearts and lungs but shared their diaphragm muscle and some anatomical structures below the diaphragm. They had one liver, one bladder, two kidneys and three legs. They each had a stomach.
“Before separation, you could think of their anatomy as two people above the rib cage, merging almost into one below the bellybutton,” said plastic and reconstructive surgeon Peter Lorenz, MD, professor of surgery, who led the reconstructive phase of the twins’ separation.
The separation team included about 50 people. By the time the twins go home, more than 100 hospital caregivers will have helped with their case, including many physicians and nurses who took care of Aida during her high-risk pregnancy and who cared for the twins as newborns.
Separation day
The girls were wheeled into the operating room shortly after 7 a.m. Dec. 6, where they were carefully anesthetized by a team of six anesthesiologists, three per twin, led by Gail Boltz, MD, clinical professor of anesthesiology, perioperative and pain medicine. Once the twins were anesthetized, the team placed central and arterial lines to enable blood transfusions and deflated the three saline-filled tissue expanders that had been used to generate new skin to help cover their separation site. The first incision was made at 11 a.m.
Erika and Eva had received comprehensive CT and MRI scans as part of the preparation for surgery, and these were used to print 3-D models of their pelvic bones and blood vessels to help plan the division. But there were still questions about details of the girls’ shared anatomy, which the team spent about an hour resolving at the beginning of the surgery.
“We had amazing information from our radiology colleagues, but even with that there were some surprises,” Hartman said. “There was only one large intestine. It appeared that it all belonged to Eva but had some blood supply from Erika, so we had to do some testing in the operating room to clarify that.” During surgery, the team also found that the girls shared a single pericardial sac around their separate hearts, and that each child had her own gallbladder.
Once the exploratory phase was complete, the team divided the twins’ liver and split their gastrointestinal and urinary tracts. The girls’ single bladder was divided and made into two bladders, and each child received a colostomy. The pelvic bones were then divided.
The biggest risk that the surgical team had anticipated prior to separation was excessive bleeding from small, diffuse blood vessels and from the pelvic bones, but fortunately the twins did not experience excess blood loss. The final incision that officially separated Eva and Erika was made by James Gamble, MD, professor of orthopedic surgery, and Matias Bruzoni, MD, assistant professor of pediatric surgery, at 4:34 p.m. Dec. 6.
For the first time, separate rooms
After the girls were separated, Eva was wheeled to an operating room across the hall, marking the first time in their lives the twins were in separate rooms. Lorenz led the team that performed Eva’s reconstructive surgery, which took until 12:30 a.m. Dec. 7. Erika’s reconstructive surgery, led by pediatric plastic and reconstructive surgeon Rohit Khosla, MD, assistant professor of surgery at the School of Medicine, was completed an hour later. Eva had enough skin from the tissue expanders to completely close her surgical site. To help complete Erika’s reconstruction, the bones from the girls’ third leg were removed, and skin and muscle from the leg were used to close Erika’s abdominal wall. The surgeons had considered keeping the leg with Erika if it was not needed for reconstruction, but it would likely not have been useful for walking because of its abnormal anatomy.
Throughout the surgery, the team used a 3-D, virtual-reality imaging system that was recently introduced at Packard Children’s. The imaging system allows the surgeons to put on 3-D glasses and view an image that can be rotated and manipulated to better see the anatomy detected in prior radiology scans. Pediatric radiologist Frandics Chan, MD, associate professor of radiology, assisted the surgeons with the new technology.
“When it became clear that we needed to use the third leg for reconstruction, Dr. Chan came in to the operating room and showed the team exactly where the blood vessels supplying the leg were located so that they could plan how to protect the blood supply to the leg,” Hartman said.
Now that Eva and Erika are separated, each child has one kidney and one leg. As the girls heal and grow, the team will assess whether any further reconstructive surgeries would be helpful for either child. “We set them up so that if everything heals well, they may not need any further surgery,” Hartman said.
The expertise of many Stanford pediatric specialists contributed to the separation’s successful outcome, with surgeons specializing in gastrointestinal, orthopedic, urologic and plastic and reconstructive surgery all contributing. “We have both the subspecialist surgeons we needed and the appropriate anesthesia and nursing expertise to take care of Eva and Erika during and after their separation,” Lorenz said. “We do high-risk surgical cases often, and our experience counts a great deal for a case like this.”
“The results are as good as we could have asked for,” Hartman concluded.
A brief look at the girls' birth:
Conjoined twins are rare. They occur in 1 in 30,000 to 1 in 200,000 births. When Aida Sandoval was referred to Packard Children’s midway through her 2014 pregnancy with Erika and Eva, the hospital’s Fetal and Pregnancy Health Program immediately brought together physicians from high-risk obstetrics, neonatology, radiology, surgery, pediatric urology, and other specialties to form an expert group that could care for Aida and both babies. Aida had high blood pressure, which further complicated an already difficult pregnancy.
“In addition to our multidisciplinary team’s very close monitoring of Aida and our vigilant evaluation of fetal health, we had to create a detailed delivery plan that included simulation of potential delivery scenarios,” said Susan Hintz, MD, professor of neonatal and developmental medicine and medical director of the Fetal and Pregnancy Health Program. After performing fetal MRI scans to investigate the babies’ anatomy, the team brought in Louis Halamek, MD, professor of neonatal and developmental medicine and director of the Center for Advanced Pediatric and Perinatal Education at Packard Children’s, who made a specialized conjoined mannequin that resembled the twins as closely as possible to facilitate realistic simulations.
“Because the girls were situated facing each other, we knew that if they were delivered prematurely and had respiratory issues, the physical constraints of how they were connected could pose challenges to successful resuscitation, including intubation,” said Hintz, who is also the Robert L. Hess Family Professor.
The team practiced potential delivery scenarios with the mannequin, including intubating, or inserting breathing tubes. Fortunately, when the girls were delivered by cesarean seven weeks early on Aug, 10, 2014, they were able to breathe without intubation, instead requiring positive pressure and oxygen via face masks. Nevertheless, Eva and Erika were fragile. They were hospitalized at Packard Children’s for their first six months of life, and then followed by several physicians as they grew big enough to be separated.


